Rheumatoid Arthritis
- Description/Cause
- Most common form of inflammatory arthropathy
- affects 0.5%-1% of general population
- twice as many women as men
- Most common and best described rheumatic case of elbow instability
- instability caused by direct weakening of ligaments from synovitis and further erosion of bone and hyaline cartilage
- instability is manifested by anterior displacement from biceps contraction
- Earliest pathologic abnormality is acute synovitis
- Primary target is synovium
- Capsular distension
- Due to hypertrophied and congested synovium
- Causes elbow pain and contracture
- patient holds elbow in flexion to decrease pain, which contributes to contracture
- Decreased elbow extension
- Prevalence/Risk Factors
- 61% of patients diagnosed with RA had radiologic evidence of elbow involvement
- only 5% of patients have RA isolated to elbow
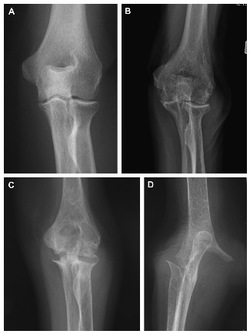
Anteroposterior elbow radiographs demonstrating the grades of rheumatoid arthritis.
a) Grade 1 osteoporosis
b) Grade 2 articular narrowing
c) Grade 3 architectural changes of the bones
d) Grade 4 gross destruction of the joint
- Signs and Symptoms
- Decreased elbow extension
- Insidious onset of morning stiffness, usually lasting longer than 30 minutes
- Posterolateral boggy swelling
- Painful clicking or snapping may be present
- Deformity, subluxation, dislocation, fracture, fragmentation and bone loss may be present with late stages of the disease
- Possible nodules, bursitis and antecubital synovial cysts
- Nodules found around elbow area
- Usually asymptomatic, but can ulcerate and become infected
- Early Stage
- Soft tissue edema
- Periarticular osteoporosis
- Middle Stages
- Proliferative granulation tissue/pannus attack joint at margins
- Narrowing joint space and periarticular bony erosions noticeable on radiographs
- Later Stages
- Inflammatory panes projects into joint and extends across joint
- Cartilage and bone damage
- Bony erosion and subchondral cysts noted on radiographs
- Varus deformity due to bone destruction
- Objective and Special Tests
- Range of Motion
- Goniometry
- Extension is often limited due to elbow flexion contractors
- Treatment and Interventions
- No cure for RA
- Goals:
- Decrease pain
- Reduce inflammation
- Delay disease progression
- Maintain long-term function of the joint
- Physical Therapy
- Educate patients on joint protection by avoiding forces that are damaging and by maintaining motion and strength
- Medications
- Disease modifying anti-rheumatic drugs (DMARDs)
- Studies suggest early introduction to DMARDs may improve long-term outcomes
- Tumor necrosis factor (TNF) inhibitors
- Intra-articular elbow steroid injections
- Short-term relief
- repeated use is not recommended
- Surgery
- Synovectomy
- Recommended for synovitis that remains uncontrolled following 6 months of treatment
- Primary Goal: pain relief by reducing synovial tissue and fluid, thus decreasing intra-articular pressure
- Distraction/Interposition Arthroplasty
- Salvage procedure consisting of interposing fascia, dermis or Achilles tendon allograft between humerus and ulna
- Limited due to often multiple joint involvement
- Goals: reduce pain and increase functional range of motion
- Total Elbow Arthroplasty
- Used on advanced stages of RA
- Contraindicated in patients with active infection
- Over 90% of post surgical patients ached pain relief, joint stability and a functional arc of motion
- Higher complication rate and infection rate than in other large joint replacements, such as hip and knee
- Early complications: wound healing problems, ulnar nerve symptoms, stiffness, heterotrophic ossification, periprosthetic fractures, and triceps insufficiency
- Late complications: aseptic loosening
References
- Studer A, Athwal G. Rheumatoid arthritis of the elbow. Hand Clinics [serial online]. May 2011;27(2):139-150. Available from: CINAHL Plus with Full Text, Ipswich, MA. Accessed June 30, 2015.
- Worthing A, Cupps T. The Rheumatic Causes of Elbow Instability. Hand Clinics [serial online]. January 1, 2008;24(Acute and Chronic Elbow Instability):79-90. Available from: ScienceDirect, Ipswich, MA. Accessed July 1, 2015.
Acknowledgements:
David Funk, Student Physical Therapist at A.T. Still University
Ethan Hunke, Student Physical Therapist at A.T. Still University
Morgan Johnson, Student Physical Therapist at A.T. Still University
Ed Nheiu, Student Physical Therapist at A.T. Still University
Lindsay Walczak, Student Physical Therapist at A.T. Still University
Last edited: July 13, 2015