Olecranon Bursitis
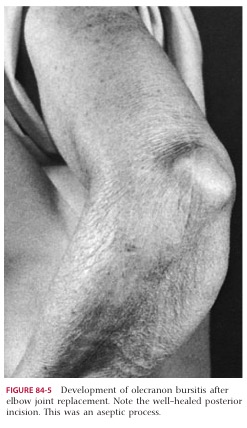
- Description/Cause
- Olecranon Bursa
- Synovium-lined sac that promotes gliding between the olecranon and overlying skin
- Susceptible to pressure, trauma, infection and inflammatory conditions
- Most common superficial bursitis
- Common cause of posterior elbow pain and swelling
- Pathology is unknown
- Idiopathic
- Traumatic
- Crystal-Induced
- Acute or Chronic
- Septic or Aseptic
- Septic becomes symptomatic earlier
- Prevalence/Risk Factors
- Individuals at risk
- Athletes who play on hard surfaces
- Occupations where individuals are subject to repetitive friction and micro-traumatic movements over the elbow ("Miner's Elbow" and "Student's Elbow")
- Individuals with Rheumatoid diseases
- Individuals with Gout
- Individuals with Staphylococcus aureus and Staphylococcus epidermis (account for 90% of all bursal infections)
- Individuals with Streptococci (accounts for 9% of all bursal infections)
- Immunodeficient individuals
- Predisposing Factors
- Overuse
- Repetitive Trauma
- Inflammatory arthropathy
- Obesity
- Prominent olecranon process or bone spur
|
- Objective and Special Tests
- Medical Imaging/Screening
- MRI
- to screen for abscesses or osteomyelitis if symptoms are severe
- hypo-intensity on T1-weighted images and variable signal intensity in T2-weighted sequences over olecranon, with concomitant surrounding soft tissue edema and contrast enhancement of bursal margins
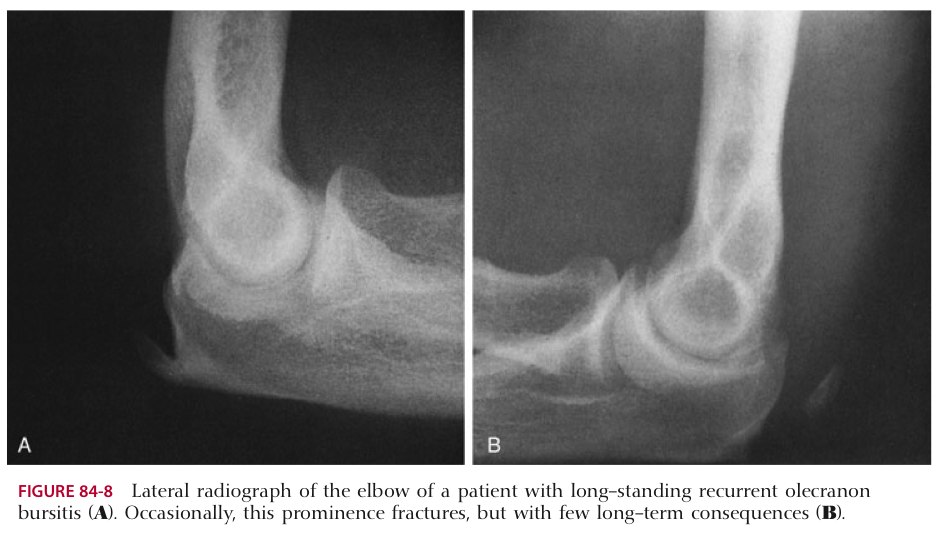
- X-Ray
- to rule-out olecranon fracture
- Microbiological investigations
- Fluid analysis
- Palpation
- Aseptic
- Commonly will observe swelling and pain over the tip of the elbow which can persist a few hours to several days
- Lump
- Painless
- Painful
- Swelling
- Hot
- Excessive Cellulitis
- Septic
- Boggy, non-tender mass over the olecranon without redness, warmth, limited range of motion, and other signs of infection
- Treatment and Interventions
- Aseptic
- Conservative Treatment
- Rest
- Ice
- Elastic Bandage
- Anti-Inflammatory Drugs
- Pain Killers
- Best approach for patients with underlying rheumatic disease, pain and swelling
- Bursal Fluid Aspiration
- Not always necessary; however, often used if conservative treatment fails
- study has shown more favorable outcomes in patients undergoing aspiration and local corticosteroid injection than in those that received just aspiration
- Corticosteroid Injection
- Long-term effects?
- Better if combined with aspiration
- Partial resection of olecranon process with no damage to bursa
- may be required for refractory cases persisting longer than three months
- Septic
- Aspiration
- Mechanical Rest
- Systemic oral or intravenous antibiotics directed by bursal fluid culture
- Recommendations
- Non-surgical management > surgical management
- based on level IV evidence
- Clinical course of aseptic bursitis is more complicated than septic bursitis
- Corticosteroid injections are associated with significant risks without improving outcome of aseptic bursitis
References
- Del Buono A, Franceschi F, Palumbo A, Denaro V, Maffulli N. Diagnosis and management of olecranon bursitis. The Surgeon [serial online]. October 1, 2012;10:297-300. Available from: ScienceDirect, Ipswich, MA. Accessed June 30, 2015.
- Kane S, Lynch J, Taylor J. Evaluation of elbow pain in adults. American Family Physician [serial online]. April 15, 2014;89(8):649-657. Available from: MEDLINE Complete, Ipswich, MA. Accessed June 30, 2015.
- Sayegh E, Strauch R. Treatment of olecranon bursitis: a systematic review. Archives Of Orthopaedic & Trauma Surgery [serial online]. November 2014;134(11):1517-1536. Available from: SPORTDiscus with Full Text, Ipswich, MA. Accessed July 1, 2015.
- All images obtained from: Morrey, B. (2009). Septic Arthritis. In The elbow and its disorders (4th ed., pp. 1056-1067). Philadelphia, PA: Saunders/Elsevier.
Acknowledgements:
David Funk, Student Physical Therapist at A.T. Still University
Ethan Hunke, Student Physical Therapist at A.T. Still University
Morgan Johnson, Student Physical Therapist at A.T. Still University
Ed Nheiu, Student Physical Therapist at A.T. Still University
Lindsay Walczak, Student Physical Therapist at A.T. Still University
Last edited: July 13, 2015